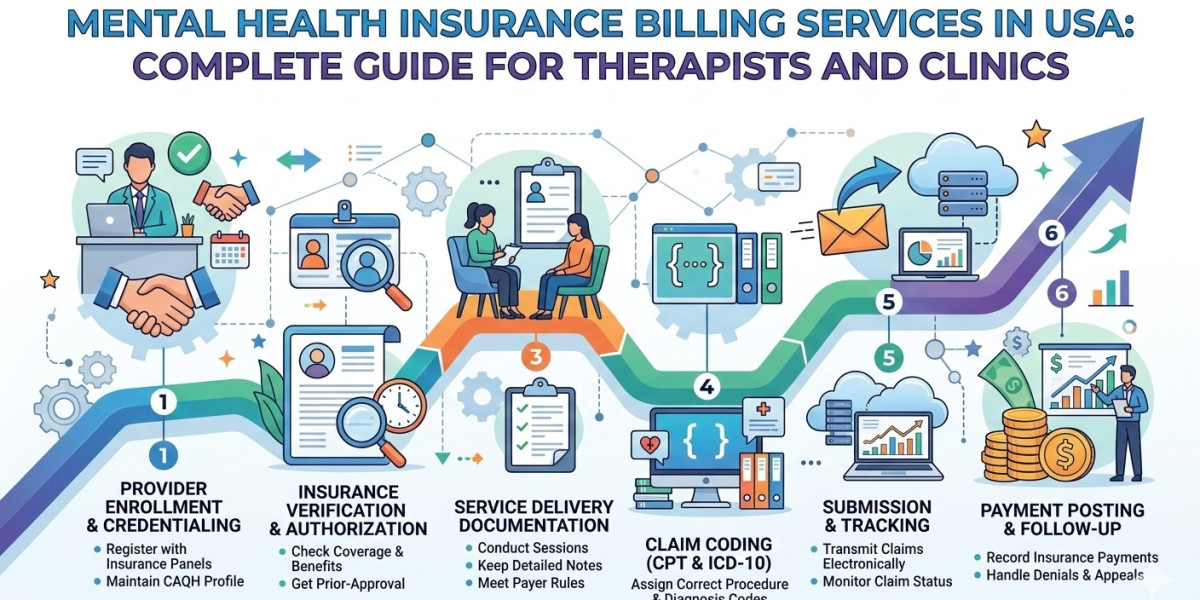
Mental health practices across the United States are expanding rapidly as demand for behavioral healthcare continues to grow. However, managing insurance claims, coding requirements, and reimbursement policies for therapy and psychiatric services can be complex and time-consuming. Many providers struggle with claim denials, documentation errors, and delayed payments.
This is where a specialized mental health billing services agency becomes essential. These agencies focus exclusively on behavioral health billing workflows, helping therapists, psychologists, psychiatrists, and treatment centers maintain a steady revenue cycle while focusing on patient care.
This guide explains how mental health billing agencies operate, why providers rely on them, and how outsourcing billing can transform the financial performance of a mental health practice.
Why Mental Health Billing Is More Complex Than General Medical Billing
Mental health billing requires a different level of expertise compared to standard medical billing. Insurance regulations, coding structures, and therapy documentation standards are highly specific to behavioral healthcare.
Key challenges include:
• Insurance authorization requirements for therapy sessions
• Complex CPT and ICD coding rules for psychiatric care
• Telehealth billing guidelines for behavioral health services
• Frequent claim denials due to documentation gaps
• Varying payer policies for counseling and therapy services
Because of these complexities, many clinics depend on a mental health billing specialist who understands payer policies and compliance requirements.
A specialized mental health medical billing solution ensures claims are coded accurately and submitted correctly the first time, reducing delays and revenue loss.
What a Mental Health Billing Services Agency Actually Does
A professional mental health billing services agency handles the entire billing lifecycle for behavioral health providers.
Typical services include:
• Insurance eligibility verification
• Therapy session coding and claim submission
• Mental health insurance billing management
• Payment posting and reconciliation
• Denial management and appeals
• Compliance monitoring
• Financial reporting and revenue analytics
These services are designed to help practices maintain stable revenue while reducing administrative workload.
A reliable mental health billing provider ensures that every claim meets payer requirements before submission, which significantly improves reimbursement rates.
Benefits of Outsourcing Mental Health Billing Services
Many clinics today prefer to outsource mental health billing services instead of managing billing internally. Outsourcing provides both operational and financial advantages.
Improved Claim Acceptance Rates
Experienced mental health billing specialist companies understand coding standards for behavioral healthcare, ensuring claims are submitted accurately.
Reduced Administrative Burden
Therapists and clinic staff can focus on patient care rather than dealing with insurance follow-ups and claim corrections.
Better Revenue Cycle Management
A professional mental health billing agency ensures claims move through the system faster, reducing delays and improving cash flow.
Compliance With Insurance Regulations
A top outsource mental health billing company stays updated on payer rules, Medicare policies, and compliance requirements.
Scalability for Growing Practices
As clinics expand, outsourced mental health billing allows providers to scale operations without hiring additional administrative staff.
Key Services Offered by Mental Health Billing Companies
Different mental health billing companies may offer varying service packages, but the core functions typically include several essential revenue cycle components.
Insurance Verification
Before appointments, billing teams verify patient eligibility and benefits to avoid claim rejections.
Accurate Therapy Coding
Behavioral health coding requires precision. A mental health billing and coding company ensures therapy services are coded according to the latest CPT and ICD guidelines.
Claim Submission and Tracking
A professional mental health billing company manages electronic claim submissions and monitors payer responses.
Denial Management
If claims are denied, billing experts investigate the issue and resubmit corrected claims.
Payment Posting
Accurate payment reconciliation ensures financial records reflect actual reimbursements from insurance providers.
These processes ensure efficient billing services for mental health therapists and clinics.
Why Mental Health Providers Choose Outsourced Billing
Many therapists and behavioral health centers rely on outsourced mental health billing because running an in-house billing department can be costly and inefficient.
Hiring a mental health billing consultant or outsourcing partner provides access to trained billing specialists without the overhead expenses of internal staff.
Outsourced mental health billing also reduces risks associated with compliance violations, billing errors, and delayed reimbursements.
For this reason, many providers actively search for the best outsource mental health billing and coding company to manage their financial operations.
Who Needs Mental Health Billing Services
A wide range of healthcare professionals rely on billing services for mental health providers to manage insurance claims effectively.
These include:
• Licensed therapists
• Psychologists
• Psychiatrists
• Behavioral health clinics
• Substance abuse treatment centers
• Counseling practices
• Telehealth therapy platforms
Each of these professionals benefits from specialized mental health medical billing services outsourcing to maintain a stable revenue cycle.
Features of the Best Mental Health Billing Agency
Choosing the best mental health billing agency requires careful evaluation. Providers should consider several important factors before selecting a partner.
Industry Expertise
A top mental health billing company should have extensive experience in behavioral health billing.
Certified Coding Specialists
Professional coders ensure therapy services are documented correctly.
Denial Management Process
Effective follow-up on denied claims improves reimbursement rates.
Transparent Reporting
Reliable mental health billing companies provide detailed financial reports and analytics.
Compliance and Data Security
Billing partners must follow HIPAA regulations and maintain secure data systems.
Selecting the best mental health billing services company ensures that billing operations remain efficient and compliant.
How Mental Health Billing Improves Revenue Cycle Performance
A structured revenue cycle plays a major role in the financial stability of healthcare practices.
With the support of behavioral & mental health billing services, providers can reduce common billing issues such as:
• Delayed insurance payments
• High claim denial rates
• Coding inaccuracies
• Untracked reimbursements
Professional billing companies for mental health use advanced systems and experienced staff to monitor each stage of the revenue cycle.
As a result, clinics often see faster reimbursements and improved financial performance.
Common Billing Errors in Mental Health Practices
Without specialized billing support, mental health practices often face several recurring billing problems.
These may include:
• Incorrect therapy CPT codes
• Missing authorization documentation
• Improper patient eligibility verification
• Incomplete claim information
• Failure to follow payer-specific guidelines
A mental health billing specialist ensures these errors are identified before claims are submitted.
Working with a professional mental health billing company significantly reduces the likelihood of revenue leakage.
How to Choose the Best Mental Health Billing Company
Selecting the best mental health billing company involves reviewing several operational factors.
Providers should evaluate:
• Experience in mental health insurance billing
• Knowledge of therapy-specific coding standards
• Transparency in pricing models
• Technology integration with EHR systems
• Client support and communication
The right partner should function as a long-term mental health billing consultant, helping providers improve financial workflows.
Many growing clinics also prefer outsourcing mental health billing and coding because it offers access to experienced specialists without increasing operational costs.
Role of Technology in Modern Mental Health Billing
Technology plays an important role in modern mental health medical billing services.
Advanced billing platforms help streamline tasks such as:
• Automated claim submission
• Electronic eligibility verification
• Real-time claim tracking
• Digital payment posting
• Financial performance reporting
These tools allow a mental health billing services company to manage billing processes efficiently while minimizing errors.
When combined with expert billing specialists, technology creates a reliable mental health medical billing solution for behavioral healthcare practices.
Conclusion
Managing the financial operations of a mental health practice requires specialized knowledge of insurance regulations, coding guidelines, and payer requirements. A dedicated mental health billing services agency provides the expertise needed to ensure accurate claims, faster reimbursements, and improved revenue cycle performance.
By partnering with experienced mental health billing provider organizations, therapists and behavioral health clinics can focus on delivering quality patient care while experts manage the complexities of insurance billing.
For providers seeking dependable billing support, 247 Medical Billing Services offers comprehensive healthcare revenue solutions including medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services. These services are designed to help healthcare organizations maintain compliance, streamline operations, and maximize reimbursement efficiency.
Frequently Asked Questions
What does a mental health billing services agency do?
A mental health billing services agency manages the complete billing process for behavioral healthcare providers, including coding, claim submission, payment tracking, denial management, and insurance follow-ups.
Why should therapists outsource mental health billing services?
Therapists choose to outsource mental health billing services to reduce administrative workload, improve claim accuracy, and ensure faster insurance reimbursements.
How do mental health billing companies reduce claim denials?
Mental health billing companies use experienced coders, verify insurance eligibility, follow payer guidelines, and monitor claims before submission to reduce denial rates.
What services are included in mental health insurance billing?
Mental health insurance billing typically includes eligibility verification, therapy coding, claim submission, payer communication, denial management, and payment posting.
How do I choose the best mental health billing agency?
To select the best mental health billing agency, providers should evaluate industry experience, compliance standards, coding expertise, reporting transparency, and customer support.
Who can benefit from billing services for mental health providers?
Psychiatrists, psychologists, therapists, counseling centers, and behavioral health clinics can all benefit from professional billing services for mental health providers to maintain an efficient revenue cycle.